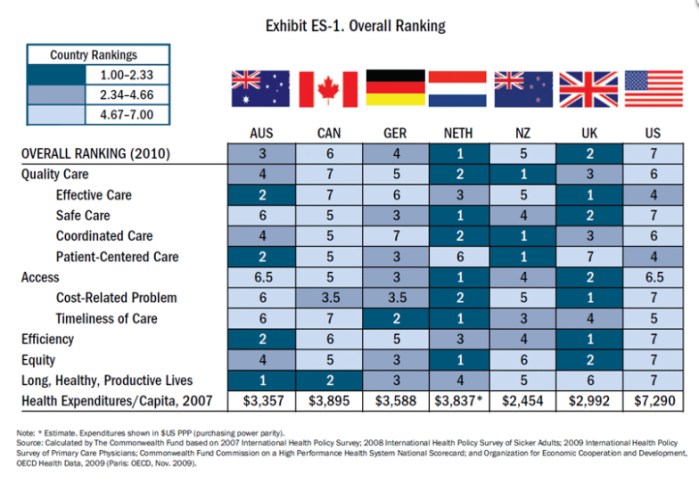
New Zealand has moved from first to fifth place in international health rankings of seven countries, carried out by the Commonwealth Fund
The slide is due mostly to issues of access, high costs preventing people from visiting doctors or filling prescriptions, safety and management of chronic illness and New Zealanders being the patients most likely to get an infection whilst in hospital. They were also in the bottom three for medication errors and being the victim of a medical mistake.
Interestingly, it was ranked last for the percentage of money spent on health administration and insurance. According to Stuff:
Labour health spokeswoman Ruth Dyson said the fall was “devastating”.
New Zealanders had worked hard to get an excellent healthcare system and were now “just watching [it] slip away”.
Government contracts held by district health boards for community-based management of chronic conditions had been cut around the country, she said.
The high infection rates were a surprise, but could be the flow-on effect of Government “penny pinching”.
It was disappointing New Zealanders were still struggling to access primary healthcare as it was crucial to early treatment and keeping people out of hospital, she said…”
Per head Australians spent US$3,357 on helathcare, Canadians US$3,895, Germans US$3,588, the Netherlands US$3,837 and Britons spent US$2,992 on health in 2007. New Zealand spent the least at US$2,454.
We can’t say that we are surprised by New Zealand’s poor showing and this is why:
New Zealand has a workforce crisis in its hospitals with specialist senior doctors being lost, there is also a shortage of cancer specialists, paediatric surgeons and radiologists and when doctors and specialists speak out about their concerns over patient safety they are censured, most of them simply resign rather than take the flack for being a whistle blower.
The average medical student in New Zealand finishes training with a debt of $75,000, forcing many of them overseas soon after graduating. Australia is their most likely destination. But money isn’t the only factor making them leave. One study found that just 25% of students believed they would be valued as employees by hospital management or the Government, something that affects their long term commitment to their country and has implications for specialist training.
261 people in Canterbury are waiting more than six months for cancer-detecting colonoscopies, raising alarm among doctors. In July 2009 the figure stood at 75 people. A private procedure costs £1,000.
The Health Ministry is allegedly among the worst performing government departments. According to a report card ranking state agencies and bosses excessive red tape, bureaucratic systems and ineffective consultation hampering a number of government departments. It placed the Health Ministry bottom for value for money overall, and said it was “struggling“ and
“really confused, with too many sections not knowing what others are doing, and doing stuff without consultation in the affected communities.”
Disgust at the plight of one hospital -Hawera – has inspired a well-placed business analyst to blow the whistle on what he sees as millions of dollars worth of financial inefficiencies and loss at the deficit-plagued Taranaki District Health Board.
Paul Anwyll left his job as a business analyst at the TDHB’s Management of Information Unit…citing “weak leadership and poor management” as reasons in his letter of resignation. An experienced auditor, the Englishman said he had identified financial problems and loss but the TDHB had refused to consider his proposal of a test study that could potentially save them millions.”
Pharmac doesn’t allow New Zealanders to access new medicines for five to 10 years after they are widely used elsewhere in the world. It waits until they are generic until they are widely used. The system keeps prices down for the Government but is criticised for restricting drug choices and delaying the arrival of some new medicines.
There was a 50% rise in complaints against pharmacists in the year to June 2009 , including 5 pharmacists who were convicted of crimes. Similar sounding and look-alike medications are ‘to blame’ for the rise. City Health Pharmacy in Palmerston North was fined $10,000 in 2008 after six drug dispensing mistakes in two years, including giving a two-year-old an anti-psychotic drug instead of cough medicine; it’s still in business. There is no compulsory bar-coding of drugs.
For a first hand account of what it’s like to work in New Zealand’s health service you may wish to read our Migrant Tale “The Health Care System is Second Rate.” Written by a nurse with over 30 years experience, she talks about resistance to change and the wastage of thousands of dollars because there is no incentive to change things.
At the time nurses in Nelson were speaking out about horrific workloads that were causing many to resign. Nurses went public because of a lack of action when they raised their concerns with the New Zealand Nurses Organisation and hospital managers.
For more read our Health and Death page
One reader of the blog left the following comment for us a week ago, if health care in New Zealand matters to you you may wish to read Gareth Morgan’s book -see a report on it here
I would like to mention that gareth morgan has a book about the nz health care system that anyone migrating for the health care ought to read, seriously.
Health Cheque: The Truth about NZ’s Health System it is called
It’s a frank book that discusses the problems with the way they rationalise care in which he states a theory that the high quality of the doctors and nurses are the only thing holding the system together.
Yet New Zealand has the highest percent of migrant doctors in the OECD, a staggering 52%
http://hpm.org/en/Surveys/The_University_of_Auckland_-_New_Zealand/15/Strategies_to_overcome_workforce_shortages.htmlsays in the review this book that:
“The New Zealand health workforce is under pressure from a number of sources. In addition to those problems that are shared by other countries – such as an increase in the proportion of part-time workers due to the feminisation of the workforce, increased demand for health services, and the aging of the health workforce – New Zealand faces major challenges from the internationalisation of health workers. It has the highest percentage of migrant doctors among OECD countries (52 percent compared with an OECD average of 36 percent) and one of the highest for nurses (OECD, 2008). **It also has one of the highest rates of outward migration of health workers. Four years after graduating, around 25 percent of NZ trained doctors are no longer registered in New Zealand and the loss increases to around one third after 9 years.**”
The doctors and nurses seem to mostly be british people who are outdoorsy migrants, or locum americans taking a working vacation, or political or crime refugess who could not get into other countries such as oz or canada. The kiwis just bugger off out of their own country and people from countries where the native language is not English are often only offered less responsible positions, in caregiving and cleaning.
The National led government has recently announced that it will be putting further pressure on the health service by giving employers the authority to make workers obtain GP sickness certificates for a single day’s sick leave from work.
“General Practice New Zealand chairwoman Bev O’Keefe said the change could put pressure on medical centres.
“The issue for general practice is how we accommodate all those people who need to claim medical certificates because they will need to be seen and assessed which means they are going to impact on what is already the heavy workload of general practice. “One thing we are not happy to do is to furnish medical certificates without seeing people because that’s just hearsay.” Another issue was people may go to work ill.”
NZ could probably get better professionals if they seriously listened to the concerns of bullying among such people.
But of course, as a Kiwi girl told me once, to my stunned silence:
“Best friends ALWAYS agree with one another!”
Oh well. “Harden the fxxk up” is great for getting through a crisis. Terrible for building a sustainable society. Horses for courses, and all that.
I have been put on the list for a simple and common enough diagnostic procedure but it will take them a year to get around to me. “Year-long waiting list”. I have a Portuguese friend (and you know Portugal is in the headlines for being hard-hit in the recession!) who was astounded at how long it would take. Matter of weeks there where he is. New Zealand doesn’t want to think of itself in the same basketcase as Ireland, Greece and Portugual, and you know? It doesn’t have to. In the sense of taking care of its citizens, it’s worse.
New Zealand is not a place where you want to become very ill, especially with something rare. T
http://www.stuff.co.nz/4535674/Review-may-widen-drug-treatment-options
Patients with rare conditions are missing out on life-enhancing drugs, with Pharmac declining more than three-quarters of funding applications last year.
Doctors and patient groups say many people do not apply to Pharmac’s exceptional circumstances scheme because applications for expensive drugs are often declined.
The Government drug-buying agency is reviewing its three exceptional circumstances schemes that consider funding drugs for patients in rare or unusual medical situations, where there are cost-savings to hospitals and for cancer patients in certain circumstances.
“It was the most horrifying, ridiculous, frustrating thing I have ever come across,” Hill said of the funding rejection.
“Somebody decides if you are worthy or not, and that’s a frustrating place to be because what makes somebody worthy and somebody else not?”
Hill said he had always been a proud Kiwi, but now felt “disgusted” with his country.
“I worked really hard for the people in this place and it’s not their fault I have got this condition, but how can they choose one person over another, and how can other countries see the value in this and others can’t?”
Only a longtime migrant in New Zealand would not laugh at the statement that Kiwis actually take “DENTAL VACATIONS IN THAILAND”. Because it is not a joke. They do. They need dental work, they go to Thailand to get it done well and cheaply, and recover on the beach with painkillers and booze!
Metiria Turai summarised many of New Zealand’s problems in the very recent Green Party response to the Key speech, and mentioned that it has third world rates of rheumatic fever resulting from from overcrowding – costs the NZ health system $10 million every year, money the system can ill afford.
http://topnews.net.nz/content/29916-nz-s-high-rheumatic-fever-rate-blamed-overcrowded-housing
And why is shared housing such a popular housing option in New Zealand? Because the housing is too expensive for many people to have their own. The young suffer very disproportionately.
New Zealand needs better universities to train their nurses. Look at Canada. They have better universities to educate their doctors and nurses, better system to self-manage medical professionals.
Other than that, I’ve seen so many New Zealanders visiting South Korea for medical tourism.